A Shot in the Arm
Vaccine clinics address patients’ fears by meeting them where they are, taking their concerns and questions seriously.
The patient had swallowed enough of his fear of the COVID-19 vaccine to come to the Armory in Washington Heights for his first shot. Still, he felt uneasy, recalls MDE student Ian Irwin, one of more than 100 Columbia Nursing students who trained to be a vaccination volunteer. “He wanted to know how the three major vaccines (Moderna, Pfizer-BioNTech, and Johnson & Johnson) compared to each other and how their clinical trials had been conducted,” Irwin says. “He wanted to know which vaccine President Joseph Biden and Vice President Kamala Harris had received. As a Black American, he was especially concerned about whether taking the vaccine would make him the subject of an experiment.”
Such questions and fears reflect those of many unvaccinated Americans—a sizable portion of whom are people of color—according to the Centers for Disease Control and Prevention (CDC). As of mid-July, for instance, only 25% of Black Americans and 31% of Hispanics were fully vaccinated, compared with 34% of white Americans. And the nation as a whole missed the vaccination target set in May by the White House: having 70% of adults receive at least one shot by July 4 (about 67% of adults had received at least one shot by that date, and the goal was achieved a month later, on August 2).
Pundits blame too-low vaccination rates on “vaccine hesitancy.” But this term does not capture the deep, collective mistrust of a health-care system that has historically discriminated against, underserved, and in other ways mistreated communities of color—and continues to do so today, say public health experts like Columbia Nursing’s Kellie Bryant, DNP, an associate professor, the assistant dean for clinical affairs and simulation, and the executive director of the Helene Fuld Health Trust Simulation Center. “Some people of color don’t trust the vaccine,” Bryant says. “They believe it has not been fully tested, they don’t trust the government because of past unethical research studies, they don’t want to be a guinea pig, or they are afraid of side effects,” she explains. To address this mistrust and increase vaccination uptake, particularly among the Black, Latinx, and LGBTQ communities in and around its Northern Manhattan neighborhood, Columbia Nursing has been conducting vigorous educational outreach, running clinics, and training a cadre of students not only how to inoculate patients but also how to provide the empathy and understanding that many need before rolling up their sleeves.

The simulation center was a perfect venue for training the volunteers.
A History of Mistreatment
Conversations about mistrust of the health-care system commonly point to the 40-year-long Tuskegee Study of Untreated Syphilis in the Negro Male, which the United States Public Health Service launched in 1932 to examine the natural course of untreated syphilis. Participants included 600 Black men, mostly poor and illiterate sharecroppers, 399 of whom had syphilis. The disease had no proven cure when the study began, and although penicillin became the standard of care in 1947, researchers withheld it as a part of the experiment, leaving dozens of men to die while infecting their wives, children, and countless others.
Nearly a century later, wide-ranging mistrust in the health-care system persists, largely because of discrimination and other barriers that fuel disparities in health and health care among communities of color and sexual and gender minorities, says Julian Watkins, MD. Watkins is a senior clinical advisor and the leader of the Immunization Justice Workgroup at the New York City Department of Health and Hygiene; he sits with Bryant and other healthcare providers of color on a committee known as the NYC Black and Latinx Providers Collective, which develops strategies for increasing vaccination rates in Black and Latinx communities. Such disparities appear in the treatment and outcomes of Black hospital patients, who are less likely than whites to receive adequate pain relief; in Black and Indigenous women, who are three to four times more likely than white women to die in childbirth, regardless of education or socioeconomic factors; and in LGBTQ individuals, who routinely face stigmatization and therefore avoid interacting with the health-care system. “Often, when LGBTQ folks go to a doctor, they’re discriminated against,” Watkins says, pointing to a growing body of legislation that allows medical providers to ask for religious exemptions from caring for people who identify as queer or trans. “They go in seeking care and end up facing a judge and jury,” he says. “This has a chilling effect when it comes to getting vaccinated,” he adds.
Barriers to COVID Testing and Treatment
The “visceral reaction to the mismanagement of health care” in their communities has played a major role in preventing people of color and other minority groups from getting vaccinated, notes Robert Fullilove, EdD, a professor of sociomedical sciences at Columbia University Medical Center and the associate dean of community and minority affairs at Columbia’s Mailman School of Public Health. “Look at how poorly we did at the beginning of the pandemic,” Fullilove says. “People needed a car just to get tested and then got turned away after standing in line for hours. When they showed up for their appointment, they had to present a bar code on their phone. What if you don’t have a phone? In Washington Heights, many folks don’t have access to the internet. Think about all the kids who did their schoolwork at McDonald’s just so they could get an internet signal.”
These structural barriers, in addition to a long history of discrimination and abuse at the hands of the medical system, have deepened people’s mistrust of the COVID vaccines and those providing them. “You have folks saying, ‘Where were you at the beginning when it was hard to get access to testing and treatment? You’ve never demonstrated that you’ve had my best interest at heart. Why should I trust you now?’” Fullilove says. “It’s not that people aren’t fully informed. It’s that the mistrust is deep.”
Because of this mistrust and other barriers, the pandemic has hit communities of color hardest, exacerbating socioeconomic inequities as well as those involving health and health care. Indeed, Black and Latinx people are both 2.8 times more likely to be hospitalized with COVID-19 than whites, while death from COVID-19 is 2.0 times more likely for Blacks and 2.3 times more likely for Latinx people than it is for whites.
Meeting Patients Where They Are
As last winter’s vaccine rollout began in New York City, Columbia Nursing seized a critical opportunity: getting shots into as many arms as possible. This was no easy task, since the initial number of people wanting the shot quickly exceeded the number of qualified vaccinators. To meet the demand, the NYC Department of Health (DOH) put out a call for volunteer vaccinators. Immediately, hundreds of Columbia students answered the call. “We initially had 200 students who wanted to help because the need was so great,” Bryant recalls.
She and her colleagues at the simulation center selected as many students as they could train—116. To qualify, students had to meet the NYC DOH requirements: completion of at least one year of clinical practice, CPR certification, and four online training modules. Then they had to successfully complete the school’s own two-hour, online training course, which included reviewing simulations about administering injections and dealing with vaccine-related medical emergencies. After completing these prerequisites, students could administer vaccines under the supervision of a nurse or nurse practitioner. In addition to preparing volunteers, Bryant and Stephen Ferrara, NP, an associate professor of nursing and the associate dean of clinical affairs, conducted webinars on COVID vaccine hesitancy for Columbia Nursing’s staff, faculty, and students.
Under Bryant’s leadership, students first administered vaccinations at the Armory in Washington Heights. “We had faculty there to supervise the volunteers, who gave vaccinations two days a week until May,” she says. By then, the students had helped to vaccinate more than 150,000 people, including Columbia, Cornell Medicine, and NewYork-Presbyterian employees. “It was such a positive experience for the students to be on the front line administering the vaccine,” Bryant says.
One of the participants in the initiative was MDE student Britt McNamara. “This is probably the only time in my life I was going to see people excited about getting a shot,” McNamara says. “We also provided patients with education associated with vaccination,” she adds. “We explained what ‘full immunity’ means, described the side effects they could expect, gave them information about taking Tylenol or Advil for pain at their injection site, and told them how to schedule their second shot,” she explains. “Having this information gave patients a little agency.”

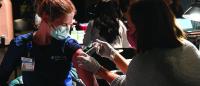
Kellie Bryant, front left, oversaw the selection and training of volunteer vaccinators.
Although some people were eager for their jab, others needed a bit of encouragement and happily accepted the t-shirts and masks that students offered at their next vaccination site: a pop-up wellness clinic in Manhattanville. At this clinic, Bryant, her students, and nurses from NewYork-Presbyterian Hospital vaccinated some 700 people—many of whom were either homeless or living in public housing. “We chose Central Harlem because it had low vaccination rates,” Bryant says. The wellness center staff took advantage of the idle post-vaccination rest period, when students and nurses observed patients for any negative reactions, to enroll interested patients in health insurance programs. “We wanted to address at least one other social determinant of health to provide some kind of lasting effect on the community,” Bryant says.
After volunteering at the pop-up clinic for four weekends, Columbia Nursing students traveled to the Harlem Children’s Zone school, where they vaccinated eligible tweens and teens. Then, to make the most of their people power—and to avoid wasting leftover vaccine—they offered remaining shots to anyone who expressed an interest. “We went out to the street to see who wanted the vaccine,” Dr. Bryant says. “We were able to find many people willing to be vaccinated.”
Bryant knows that the decision to receive the vaccine is a personal one and that a percentage of individuals will choose not to, which troubles many public health officials, given the current increase in COVID-19 cases that the Delta variant is likely causing. Yet eliciting and understanding people’s concerns regarding the vaccine is critical, she says. “There were early adopters who couldn’t wait for the vaccine, others who took a wait and see approach, and some who did not want the vaccine for various reasons. We’ve had people who were still unsure about the vaccine as they sat in the chair,” she says. “The best we can do is meet them where they are, find out why they don’t want the vaccine, and address their specific concerns.”
One way of doing this is to acknowledge people’s concerns about the rapid development of the vaccine. “We tell patients, ‘Yes, atrocities happened and were horrible, but because of those unethical studies, a lot of checks and balnces have been built into research to prevent them from happening again,’” she says.

Bryant has presented more than 20 vaccine education webinars to state and national organizations (like the New York State Black Caucus and the National Association for the Advancement of Colored People [NAACP]); has conducted community forums with Fullilove, including one at the Williamsbridge branch of the NAACP; and sits on the National Nurse-Led Care Consortium’s Vaccine Confidence Advisory Committee. She tries to calm patients’ fears by describing her own positive experience with the vaccine. She also emphasizes that the vaccine research trials included people from all racial and ethnic backgrounds. “I provide factual knowledge to address patients’ concerns directly,” she says. “I don’t push the vaccine on people, and I don’t use fear tactics to convince them to receive the vaccine.”
Columbia Nursing student Irwin took a similarly empathic approach with his willing but nervous patient. “I told him that I had gotten the Pfizer vaccine, which is what he was going to receive that day,” Irwin explains. “I described my experience and that of people I know. Then I walked him through all of the potential side effects and complications, their likelihoods, and what I knew about the studies and efficacy rates of the various vaccines,” he says. Together, he and his patient even looked up which vaccines President Biden and Vice President Harris had received (Pfizer for Biden, Moderna for Harris).
“My taking his concerns seriously and addressing them to the best of my ability in a calm, non-judgmental manner,” says Irwin, “was enough for him to feel comfortable with receiving the vaccine that day.”
This article originally appeared in the Fall 2021 issue of Columbia Nursing magazine.

